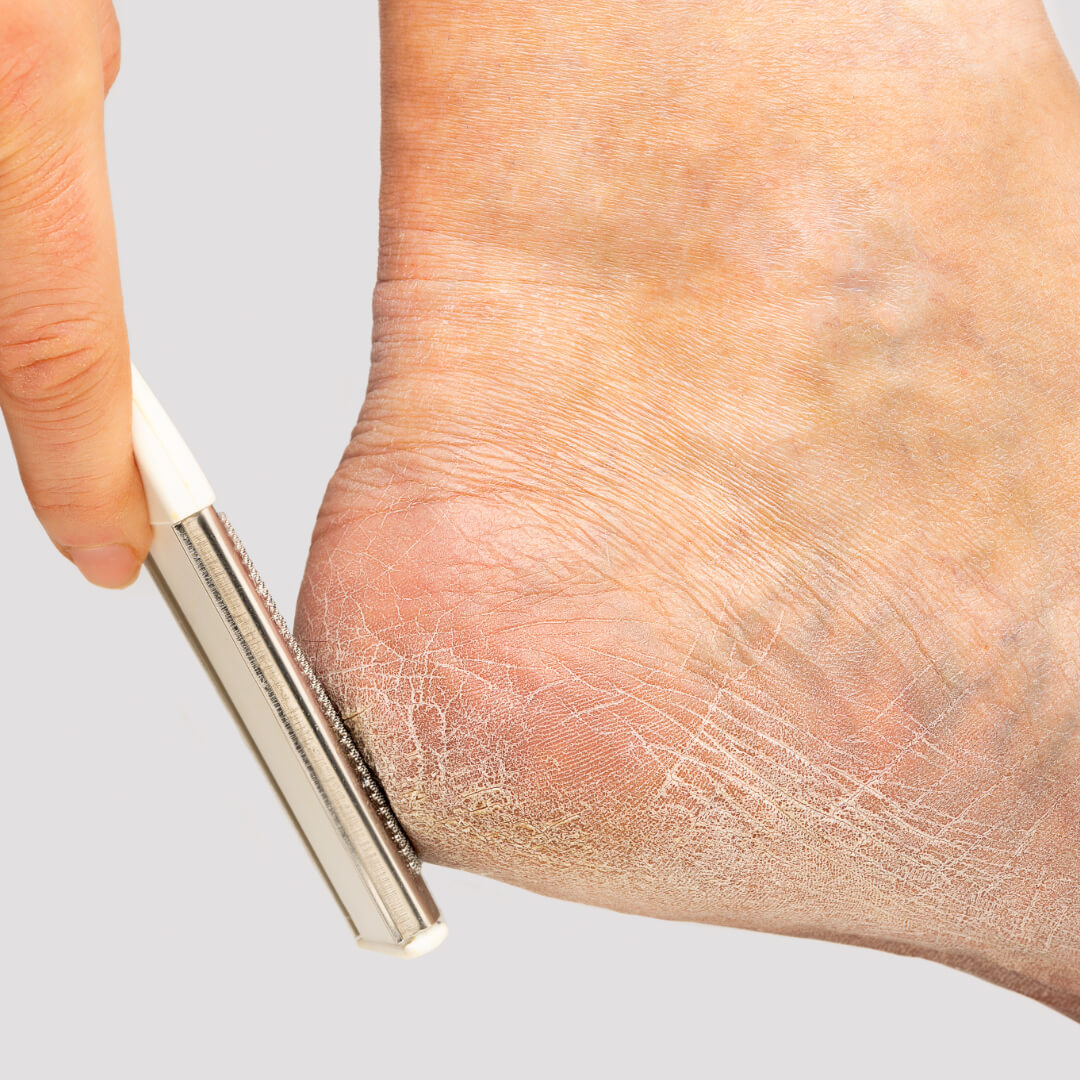
Are you struggling with cracked heels? If you have diabetes, you may be at a higher risk for this common foot problem. In fact, diabetes can play a significant role in exacerbating the condition of cracked heels. This hidden connection between diabetes and cracked heels is something that many people may not be aware of.
Understanding the connection between diabetes and cracked heels is essential for those with diabetes to take preventive measures and effectively manage their foot health. By seeking proper medical guidance, regular foot care, and appropriate treatment, individuals with diabetes can minimize the risks associated with cracked heels and maintain healthy and pain-free feet.
Understanding the link between diabetes and cracked heels
Diabetes can lead to an array of foot problems, including nerve damage and poor blood circulation. Both of these conditions can contribute to the development of cracked heels. Nerve damage, also known as diabetic neuropathy, can cause a loss of sensation in the feet, making it easier for cracks to develop without your knowledge. Without proper intervention, these cracks can worsen and become painful, increasing the risk of infection. Additionally, reduced blood flow to the feet can slow down the healing process, making it difficult for cracked heels to heal properly. Get a step-by-step guide to treating cracked and bleeding heels before they worsen — especially important for those managing diabetes.
Why are diabetic individuals more prone to developing cracked heels?
There are several factors that contribute to the increased risk of cracked heels in individuals with diabetes. One of the main reasons is the effect of high blood sugar levels on foot health. When blood sugar levels are consistently elevated, it can lead to a condition called diabetic neuropathy. Diabetic neuropathy affects the nerves in the feet, causing a loss of sensation and making it difficult to detect foot problems like cracked heels.
In addition to nerve damage, individuals with diabetes often experience poor blood circulation. High blood sugar levels can damage blood vessels, leading to reduced blood flow to the extremities, including the feet. When blood flow is compromised, it becomes harder for the body to heal wounds, including cracked heels. As a result, cracked heels in diabetic individuals may take longer to heal and are more prone to infections.
The impact of high blood sugar levels on foot health
Maintaining stable blood sugar levels is crucial for overall diabetes management, including foot health. High blood sugar levels can contribute to the development and progression of foot problems, including cracked heels. When blood sugar levels are consistently elevated, it can lead to nerve damage, poor blood circulation, and impaired wound healing.
To reduce the impact of high blood sugar levels on foot health, it's important for individuals with diabetes to closely monitor their blood sugar levels and follow their healthcare provider's recommendations for managing diabetes. By keeping blood sugar levels within a target range, individuals can minimize the risk of complications, including cracked heels.
Complications of cracked heels in diabetic patients
Cracked heels can pose significant complications for individuals with diabetes. The open cracks in the skin can serve as an entry point for bacteria and fungi, increasing the risk of infections. In diabetic individuals, infections can be more severe and difficult to treat due to compromised immune function and impaired wound healing.
If left untreated, infections in cracked heels can lead to more serious complications such as cellulitis, abscesses, and even diabetic foot ulcers. Diabetic foot ulcers are deep sores that can develop when a wound fails to heal properly. These ulcers can become infected and may require intensive medical treatment, including antibiotics, wound care, and, in severe cases, even amputation.
Tips for preventing and managing cracked heels in individuals with diabetes
Prevention and proper management are key when it comes to cracked heels in individuals with diabetes. Here are some tips to help prevent and manage cracked heels:
- Maintain proper foot hygiene: Wash your feet daily with lukewarm water and mild soap. Gently pat your feet dry, paying close attention to the areas between the toes.
- Moisturize regularly: Apply a rich moisturizer or foot cream to your feet daily, focusing on the heels. Avoid applying moisturizer between the toes, as it can create a moist environment that promotes fungal growth.
- Avoid excessive soaking: Prolonged exposure to water can strip the skin of its natural oils, making it more prone to dryness and cracking. Limit your foot soaking time to no more than 10 minutes, and always remember to thoroughly dry your feet afterward.
- Wear appropriate footwear: Choose shoes that fit well and provide adequate support. Avoid open-back shoes or sandals that can increase pressure on the heels.
- Protect your feet: Use cushioned insoles or heel cups to reduce pressure on the heels. If necessary, consider wearing protective footwear, such as diabetic shoes or custom orthotics, to minimize the risk of developing foot problems. Ask a family member to inspect your feet if you have difficulty seeing the bottom of your feet.
- Regularly inspect your feet: Check your feet daily for any signs of cracks, redness, swelling, or other abnormalities. If you notice any changes, consult your healthcare provider for further evaluation and treatment.
- Trim your toenails: Trim your toenails straight across, avoiding curved edges that can contribute to ingrown toenails. If you have difficulty trimming your nails, consider seeking professional help from a podiatrist.
- Avoid walking barefoot: Always wear shoes or slippers, even indoors, to protect your feet from potential injuries.
- Maintain a healthy lifestyle: Proper diabetes management, including maintaining stable blood sugar levels, eating a balanced diet, and engaging in regular physical activity, can contribute to overall foot health.
Importance of regular foot check-ups for diabetic patients
Regular foot check-ups are essential for individuals with diabetes to monitor their foot health and detect any potential problems early on. During a foot check-up, a healthcare provider, such as a podiatrist, will examine your feet, assess your circulation and nerve function, and provide guidance on proper foot care.
By scheduling regular foot check-ups, you can stay proactive in managing your foot health and address any concerns before they escalate. Your healthcare provider can also provide information on specific measures to prevent and manage cracked heels based on your individual needs and circumstances.
Treatment options for cracked heels in diabetic individuals
If you already have cracked heels, it's important to seek appropriate treatment to prevent complications and promote healing. Treatment options for cracked heels in diabetic individuals may include:
- Topical moisturizers: Applying a rich moisturizer or foot cream to cracked heels can help soften the skin and promote healing. Look for products specifically formulated for diabetic foot care with urea. Urea can both draw water in the skin and exfoliate dead skin buildup. The American Academy of Dermatology recommends that diabetic patients use a cream containing 10% to 25% urea to heal cracked heels.
- Debridement: In cases where the cracks are severe or accompanied by calluses, a healthcare provider may recommend debridement. Debridement involves removing the dead or thickened skin to allow healthy skin to regenerate.
- Antibiotics: If an infection is present or suspected, your healthcare provider may prescribe antibiotics to treat the infection and prevent it from spreading.
- Offloading: Offloading refers to the use of custom orthotics or special footwear to relieve pressure on the cracked heels and promote healing. Your healthcare provider may recommend offloading devices based on the severity of your condition.
- Wound dressings: For deep or non-healing cracks, your healthcare provider may apply specialized wound dressings to facilitate healing and prevent infection.
It's important to note that treatment options may vary depending on the severity of the cracked heels and individual circumstances. Always consult your healthcare provider for personalized treatment recommendations.
A Rapid Healing Cream for cracked heels and diabetes
SkinIntegra’s Rapid Crack Repair Cream is a novel repair moisturizer that was specifically formulated to help rapidly restore cracked heels in people with diabetes. Its patented composition is the result of research into all the components of a healthy skin barrier. For that reason, it includes the essential moisturizing and lipid ingredients naturally found in a healthy skin barrier such as urea, lactic acid, hyaluronic acid for moisturizers and essential fatty acids, natural oils and ceramides for lipids.
In a clinical study, 100% diabetic subjects with dry, cracked skin showed improvement after just one day.
Rapid Crack Repair Cream is free of common skin irritants which can cause a reaction and slow the natural healing process in diabetic skin such as fragrances, dyes, parabens and other harsh preservatives, petroleum-based ingredients, and phthalates.

Conclusion: Taking care of your feet is crucial for overall diabetes management
Cracked heels can be a common and troublesome problem for individuals with diabetes. The hidden connection between diabetes and cracked heels highlights the importance of foot care in diabetes management. By understanding the link between diabetes and cracked heels, individuals with diabetes can take proactive steps to prevent and manage this condition.
Maintaining stable blood sugar levels, practicing proper foot hygiene, wearing appropriate footwear, regularly inspecting your feet, and seeking regular foot check-ups are all essential components of a comprehensive foot care routine. By taking care of your feet, you can minimize the risks associated with cracked heels and maintain healthy, pain-free feet.
Remember, diabetes management is a lifelong commitment, and your healthcare provider is your best resource for personalized advice and guidance. By working together, you can effectively manage your diabetes and prioritize your foot health for a better quality of life.