If you live with diabetes, caring for your feet isn’t just about comfort — it’s about preventing serious complications that can affect your health and independence. One of the most common issues people with diabetes face is foot calluses — thickened, hardened areas of skin that can lead to infections or ulcers if not managed carefully.
In this comprehensive guide, we’ll explain why diabetic foot calluses form, how to manage them safely, and what treatments — both at home and with your podiatrist — are most effective. Whether you’re newly diagnosed or have been managing diabetes for years, understanding how to care for your feet is essential for maintaining mobility and avoiding complications.
What Are Diabetic Foot Calluses?
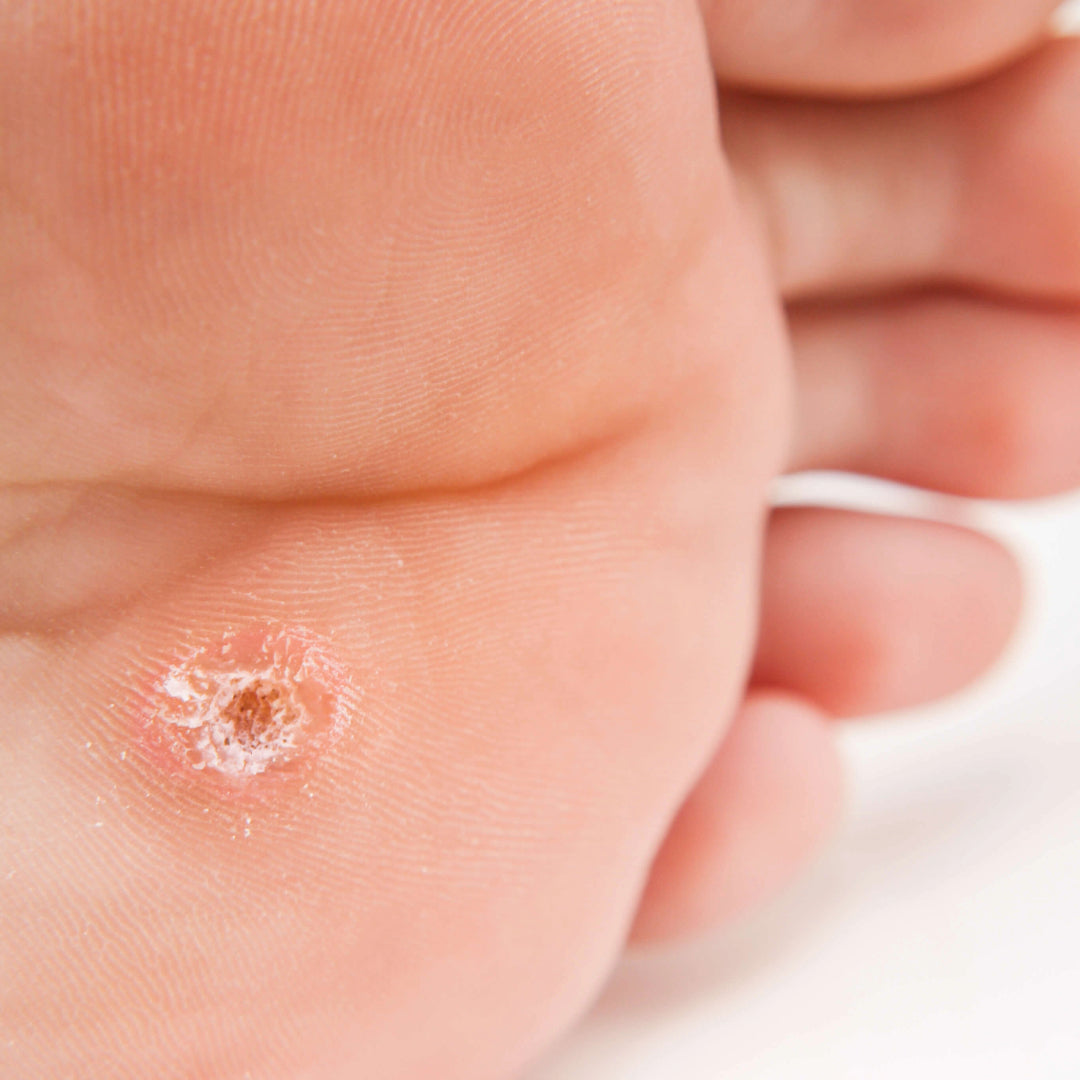
Calluses are areas of thick, dry skin that form in response to pressure or friction. On the feet, they commonly develop on weight-bearing areas like the heels, the ball of the foot, or over bony deformities like bunions or hammertoes.
For people with diabetes, calluses are more than just a cosmetic concern. They can:
-
Increase localized pressure
-
Mask developing wounds underneath
-
Crack and open the door to infection
-
Lead to ulcers, especially in those with neuropathy or poor circulation
Because diabetes can reduce sensation in the feet (a condition called peripheral neuropathy), calluses may go unnoticed until they become a bigger problem. That’s why proactive care is so important.
What Causes Calluses in People With Diabetes?
The root cause of most foot calluses is excessive pressure. In people with diabetes, this pressure is often magnified by other risk factors:
1. Peripheral Neuropathy
Nerve damage reduces the foot’s ability to sense irritation. Without feedback from pain or discomfort, a person may continue walking in a way that adds pressure to one spot — allowing a callus to build unnoticed.
2. Poor Circulation (Peripheral Artery Disease)
Reduced blood flow slows healing and thins the skin, making it more vulnerable to breakdown under calluses.
3. Foot Deformities
Conditions like hammertoes, bunions, or high arches can create uneven pressure points that lead to repeated friction and callus formation.
4. Improper Footwear
Shoes that are too tight, too loose, or lack support can cause abnormal pressure patterns — especially when combined with neuropathy.
5. Obesity
Excess body weight increases stress on the feet and can accelerate callus formation, especially in areas that already bear pressure.
Why You Should Never Ignore a Callus
Many people are tempted to self-treat foot calluses with over-the-counter tools or products — or worse, ignore them entirely.
But for people with diabetes, even a simple callus can turn into a serious wound.
-
Calluses can disguise ulcers forming underneath.
-
Cracked calluses can introduce bacteria into deeper layers of skin.
-
Infections from untreated ulcers can lead to hospitalizations — and in some cases, amputation.
Staying ahead of callus development is a crucial part of diabetic foot care. The goal isn’t just removing them — it’s preventing them from forming in the first place.
Home Care: What You Can Do Safely
If you have diabetes, foot care begins at home — but it must be done carefully and with professional guidance.
Here are safe, daily practices to help reduce your risk:
1. Keep Feet Clean and Dry
Wash your feet daily with mild soap and lukewarm water. Gently pat them dry — especially between the toes. Moisture trapped between toes can lead to fungal infections.
2. Moisturize (But Avoid Between the Toes)
Dry skin increases the risk of cracks. Use a diabetic-friendly cream to hydrate your feet, avoiding fragranced or petroleum-based products. Don’t apply lotion between your toes.
3. Wear Supportive, Properly Fitted Shoes
Avoid high heels, narrow toe boxes, or shoes without arch support. Opt for footwear designed for people with diabetes — wide, cushioned, and breathable.
4. Use Protective Padding
If you have a callus-prone area, use non-medicated cushioning pads to reduce pressure. Avoid medicated corn or callus removers containing salicylic acid. Salicylic acid is contraindicated for diabetic skin because it can break down healthy skin and lead to ulceration.
5. Inspect Feet Daily
Check for any signs of redness, swelling, skin breakdown, or pain. Use a mirror or ask for help if you can’t see the bottoms of your feet.
Safe pedicure tips for people with diabetes.
When to See a Podiatrist
Even with good home care, regular visits to a podiatrist are essential. They can help identify pressure points early, safely remove calluses, and provide custom recommendations.
Professional treatments may include:
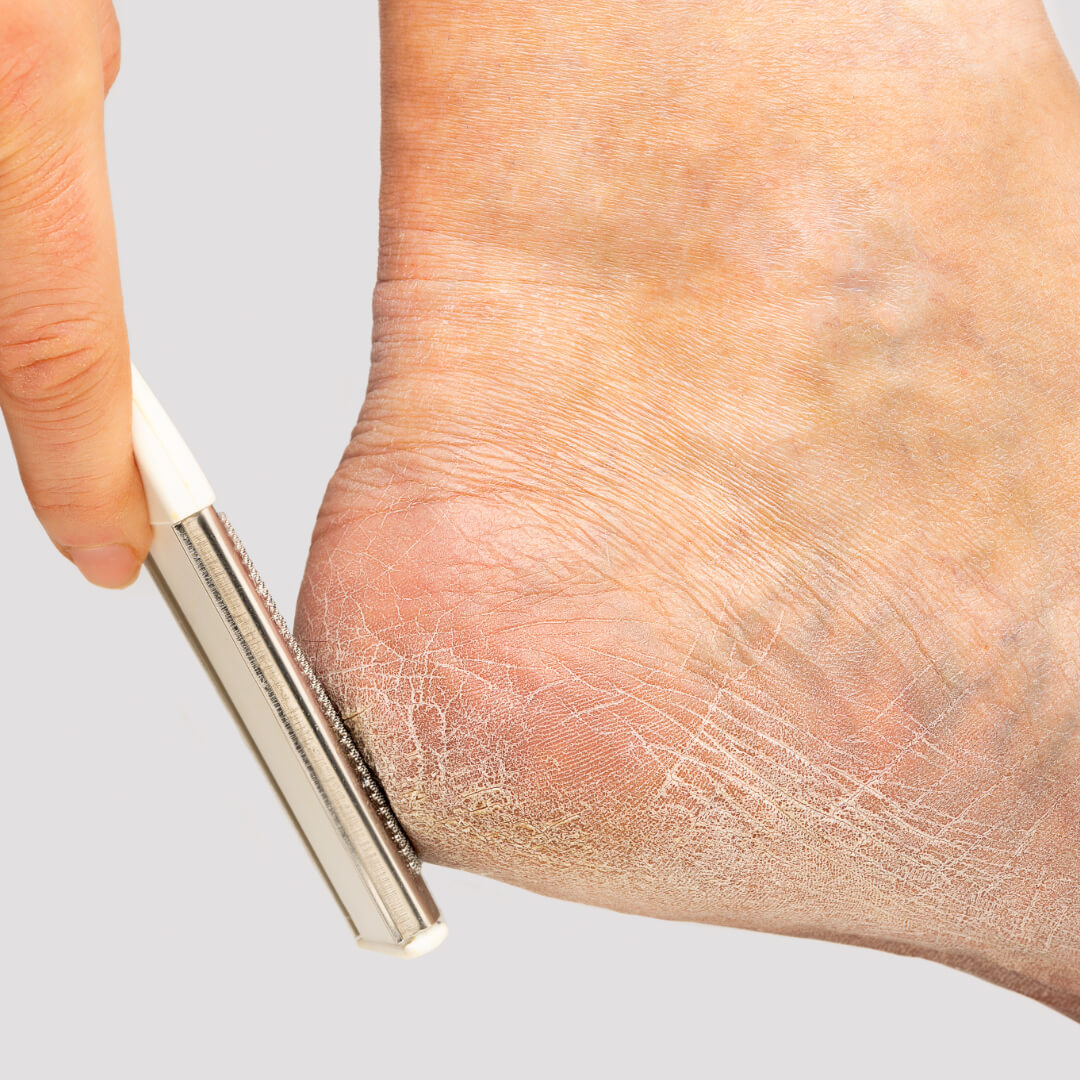
1. Debridement
Your podiatrist can gently remove the thickened skin using sterile tools — reducing pressure and helping prevent skin breakdown.
2. Custom Orthotics
These inserts are tailored to your feet and help redistribute pressure more evenly, reducing the chance of callus formation.
3. Offloading Devices
Special shoes or boots can temporarily shift weight off callused or ulcerated areas to promote healing.
4. Wound Care
If an ulcer has developed under or around a callus, proper wound care is crucial — including dressings, debridement, and infection prevention.
What to Do After Callus Debridement
After callus debridement — the clinical removal of thickened, keratinized skin — many diabetic patients experience quick recurrence due to ongoing pressure, neuropathy, or impaired healing.
A 2020 study found that 84% of diabetic patients had callus recurrence within one month, even with therapeutic footwear. That’s why what happens after debridement is just as important as the procedure itself.
Why Diabetic Skin Needs Special Attention
Diabetic skin tends to be drier, more fragile, and slower to repair than healthy skin due to microvascular compromise and reduced sebaceous activity. Following debridement, this compromised skin is more vulnerable to:
-
Cracked heels and fissures
-
Infection
-
Delayed re-epithelialization
That’s why barrier restoration — using evidence-backed ingredients like urea, ceramides, lactic acid, and hyaluronic acid — is critical to protect and hydrate the skin. Moisturizers should be non-occlusive, free of fragrance and petroleum, and optimized to improve elasticity and prevent fissure recurrence.
Learn more about barrier repair for diabetic foot care.
Key Post-Care Steps:
-
Rebuild the Skin Barrier: Moisturizing with a barrier-repair cream like SkinIntegra helps support healing and reduce re-thickening.
-
Continue Offloading Pressure: Ensure footwear and gait support remain consistent.
-
Hydrate the Skin Daily: Dry, fragile skin is more prone to cracking and fissures.
-
Avoid Irritants: Skip petroleum-based or fragranced lotions that can disrupt healing.
A Targeted Solution: SkinIntegra Rapid Crack Repair Cream

SkinIntegra’s patented Rapid Crack Repair Cream was developed specifically for diabetic skin. Its formula is precisely calibrated to address the two key challenges of managing diabetic foot calluses: exfoliating hardened buildup and restoring a compromised skin barrier.
What Makes SkinIntegra Different?
-
Exfoliating and moisturizing ingredients
-
Urea (25%): A powerful yet skin-friendly keratolytic that softens and breaks down thickened skin
-
Lactic acid: Gently loosens and exfoliates dry surface layers
-
Hyaluronic acid: Attracts and retains moisture to improve hydration and texture
-
These ingredients work synergistically to reduce build-up and help prepare the skin for barrier repair. How to safely exfoliate diabetic skin.
-
Barrier-restoring ingredients
-
Ceramides
-
Essential fatty acids
-
Natural plant oils
These components mimic the natural lipids of healthy skin, helping rebuild the barrier, reduce transepidermal water loss, and protect against further breakdown.
SkinIntegra’s formula is also:
-
Free from fragrances, dyes, parabens, phthalates, petroleum derivatives, and other known irritants
-
Safe for daily use on diabetic skin
-
Clinically tested: In a study, 100% of participants with diabetes and dry, cracked feet showed improvement after just one day
Explore the product → (https://skinintegra.com/products/rapid-crack-repair-cream)
Best Practices for Prevention
Preventing calluses is more effective — and safer — than treating them once they’ve formed. Here’s how to protect your feet every day:
|
Best Practice |
Why It Matters |
|
Visit a podiatrist regularly |
Identify pressure spots early and prevent ulcers |
|
Inspect feet daily |
Catch small issues before they escalate |
|
Wear appropriate shoes |
Reduces abnormal pressure |
|
Use non-irritating moisturizers |
Keeps skin supple and resilient |
|
Control blood sugar levels |
Improves healing and circulation |
|
Stay active |
Promotes blood flow and mobility |
|
Avoid walking barefoot |
Prevents injuries and infections |
When to Seek Immediate Medical Help
Contact a podiatrist or healthcare provider promptly if you notice:
-
Redness, swelling, or pus near a callus
-
A wound that does not heal within 7 days
-
Increased pain, burning, or numbness
-
Warmth or discoloration in the foot
-
Sudden changes in sensation or appearance
Early treatment helps avoid serious outcomes like infection, hospitalization, or amputation.
How to treat cracked heels that bleed.
Frequently Asked Questions (FAQ)
What’s the difference between a callus and a corn?
Calluses are large, thick areas of skin that usually develop on the soles of the feet. Corns are smaller, often harder, and appear on or between the toes. Both result from pressure or friction.
Is it safe to use a pumice stone?
Only under the guidance of your healthcare provider. Even minor abrasions can lead to serious wounds in people with diabetes.
Can diabetic calluses go away on their own?
They may reduce with proper pressure relief, moisturizing, and improved footwear — but it’s important to have them monitored professionally.
Do calluses always lead to ulcers?
No, but they are a known risk factor. Calluses can hide ulcers beneath them or crack and lead to infection.
Why should people with diabetes avoid salicylic acid?
Salicylic acid can damage healthy tissue, especially in people with impaired healing. It increases the risk of skin breakdown and ulcers in diabetic feet.
What’s the best cream for cracked heels after debridement in diabetic patients?
Use a non-irritating cream with urea and barrier-repair ingredients like ceramides and hyaluronic acid. Avoid petroleum-based products and fragrances.
Take Control of Your Foot Health
Diabetic foot calluses can be safely managed — and often prevented — with a combination of self-care, smart products, and professional support. By staying vigilant, using the right treatments, and partnering with your podiatrist, you can protect your feet and maintain your mobility.
Make foot care a non-negotiable part of your diabetes management plan.
Shop SkinIntegra Rapid Crack Repair Cream
Clinically backed, barrier-restoring care for dry, cracked, or callused diabetic feet.
Shop now → (https://skinintegra.com/products/rapid-crack-repair-cream)